Diagnosed during pregnancy with spina bifida, chromosomal abnormalities, and hydrocephalus, young Noah Wall has defied predictions from the British medical community.
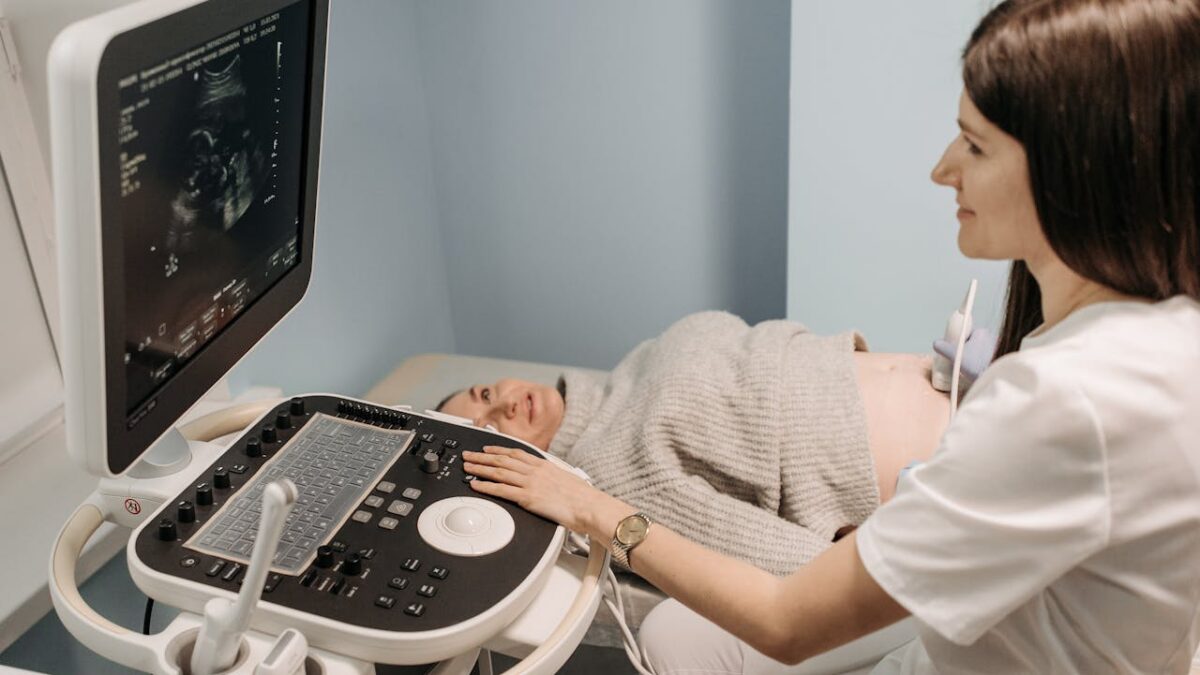
Roughly midway through pregnancy, during a 20-week scan, Shelly and Rob Wall of Cumbria, England, were told that their son Noah had spina bifida, a birth defect in which the spinal cord doesn’t fully close. Damage to the spinal cord and nerves can result. While health outcomes vary depending on the type and severity of the condition, physical and intellectual disabilities can vary from mild to severe and include paralysis of the legs.
Noah’s parents were later informed that he had hydrocephalus, a condition involving an abnormal accumulation of cerebrospinal fluid in the brain. On five separate occasions during the pregnancy, doctors advised Shelly and Rob to terminate their son, Noah. The Walls say their doctors projected that their son would be severely disabled both mentally and physically and potentially unable to see, hear, and speak.
When Shelly went in for Noah’s birth, the hospital placed a non-resuscitation order on him. She says it “was an amazing day” and “we waited with bated breath.” Noah gave a loud and strong cry announcing his birth. An initial scan showed Noah’s brain was at 2 percent of a newborn’s brain. His latest scan at age three astoundingly reflects 80 percent of a child’s brain.
Celebrating his seventh birthday this March, Noah continues to spread hope with his effusive joy. He visits and takes gifts to children in the hospital where he stayed and updates his former doctors. His parents share their story of enduring love and perseverance against pressures to end Noah’s life.
Although paralyzed from the waist down at birth, Noah has been learning to move his legs. He hopes one day to both walk and even surf. His care has led the family to an Australian clinic where Noah had an assessment in the emerging field of neurophysics.
Noah’s mom, Shelly, now also advocates for increased awareness about the importance of early folic acid intake for pregnant moms and women hoping to conceive. Folic acid, a form of vitamin B, aids in proper neural tube development as a baby grows. The neural tube in an embryo develops into the baby’s brain and spinal cord and tissues enclosing them.
Since spina bifida is a birth defect where the spinal cord doesn’t fully close, maternal folic acid intake during (and before) pregnancy has been shown to reduce the risk of spina bifida as well as the defect anencephaly—also caused by a neural tube defect. Encouraging folic acid intake through both prenatal and preconception education is a critically important prevention initiative.
Innovative prenatal surgeries also show incredible promise for babies diagnosed in utero with spina bifida and other birth defects. As a new paper entitled “The Perinatal Revolution,” co-authored by two Charlotte Lozier Institute scholars and a colleague, highlights a major reason more parents should be hopeful from a recent study.
Myelomeningocele is spina bifida in its most severe form. Not only did the research demonstrate the effectiveness of prenatal surgery, but it also found that when performed earlier in pregnancy (before 26 weeks) babies fared better. The outcomes were so positive, they interrupted the study so treatment wouldn’t be denied to babies who were to receive standard postnatal surgery. Their findings were published in the New England Journal of Medicine.
According to the U.S. Centers for Disease Control and Prevention (CDC), about 1,645 babies are born with spina bifida each year in the United States According to EUROCAT data, in the United Kingdom in 2016, a total of 53 babies were born with this condition, another 90 were lost to induced abortion, and four more babies died naturally.
Officials with the British National Health Service (NHS) announced in late 2018 that in utero spinal surgery for some unborn babies diagnosed with spina bifida will be made available in England for the first time in April 2019. It is surmised that the NHS will determine which babies may undergo the surgery and receive care.
In-Utero Surgery Helped Elouise Simpson
Elouise Simpson, a baby girl who received one of the pioneering spina bifida surgeries in the womb at University College Hospital in London in February, was born on April 1, and has now gone home with her parents. Bethan Simpson, Elouise’s mom and a mental health nurse, said she and her husband were advised to terminate their daughter following the spina bifida diagnosis.
But “I couldn’t justify terminating a child I could feel kicking,” she said. Little Elouise has shown no signs of spina bifida since birth and the in utero surgery has been deemed a success.
Stories like Noah Wall’s indicate that medical projections following a serious diagnosis during pregnancy are not always correct. The courage and love Noah’s parents demonstrated to fight to give their little boy a chance at life, despite the odds and contrary to the medical advice provided seven years ago, should encourage parents who receive such a serious diagnosis. The family interview on “Good Morning Britain” recounting their journey has endeared Noah and his parents to the public as an inspiration for hope and life.