A terminally ill child’s death should not be determined by a panel of doctors and a judge. Parents should have a say in the decision to maintain life-extending care. But in Texas, Fourth District Court of Appeals Chief Justice Sandee Bryan Marion went along with the determination of doctors at Cook Children’s Medical Center in Fort Worth to pull life support from 11-month-old Tinslee Lewis, despite her family’s wishes to keep her alive.
The Jan. 2 ruling was made based on arguments during a Dec. 12, 2019, hearing. Tinslee Lewis’s family intends to appeal the decision.
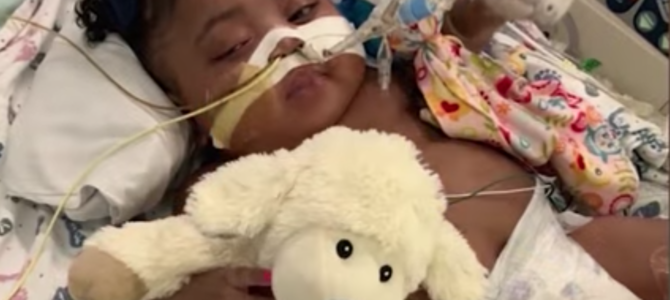
Tinslee was born in February 2019 with a host of medical ailments. She was premature and suffered from Ebstein’s anomaly, a serious heart defect, chronic lung disease, and high blood pressure. Tinslee has been breathing with the help of a ventilator since July, when she went into respiratory arrest, and is deeply sedated and medically paralyzed. Her mother, Trinity Lewis, maintains hope.
Doctors in Texas possess the legal right to determine when a patient’s life ends because of the Texas Advanced Directives Act, passed in 1999. The law requires that before physicians can terminate life support, an ethics or medical committee must vet their decision. The patient is informed at least 48 hours in advance about the meeting to end his life, and receives the information in writing. The patient and his family then have 10 days to transfer to a facility where he won’t be removed from life support, should he so desire.
Courts, Doctors, and Family Dispute Tinslee Lewis’ Care
After an October Ethics Committee meeting, doctors at the Cook Children’s Medical Center invoked the “10-day rule,” wherein they determined they can remove life support, regardless of what the patient’s family wants. In this case, Tinslee’s mother desperately wants her baby to live.
A temporary restraining order was filed to prohibit the removal of care, but it expired Dec. 10. The family tried to find a different facility that wouldn’t remove Tinslee from life support, but none could offer further life extension, and the case went to court for a temporary injunction hearing Dec. 12.
Typically, the process of ending life-extending care does not reach the court system. Families and doctors are usually able to come to an agreement about the best course of action, which is especially difficult for a mother to a baby who hasn’t even reached her first birthday. If the family cannot find adequate placement for their loved one, the hospital may cease life-extending care. Lewis is trying to keep Cook Children’s from terminating Tinslee’s ventilator while the mother seeks an appeal of Judge Marion’s decision.
Texas Right to Life advocates for continuing care, and Fort Worth Catholic Diocese Bishop Michael F. Olson has offered to help obtain care for Tinslee at a Catholic hospital. Texas Gov. Greg Abbott and Attorney General Ken Paxton issued a joint statement saying, “The state will continue to support Ms. Lewis’ exhaustion of all legal options to ensure that Tinslee is given every chance at life.” The AG’s office said it would ensure Tinslee’s right to life all the way to the Supreme Court.
After Marion’s ruling, the doctors released a statement that said, “Our medical judgment is that Tinslee should be allowed to pass naturally and peacefully rather than artificially kept alive by painful treatments. Even with the most extraordinary measures the medical team is taking, Tinslee continues to suffer. To keep her alive, doctors and nurses must keep her on a constant stream of painkillers, sedatives, and paralytics.”
The statement continued, “As a result, Tinslee is paralyzed at all times. She currently is suffering from severe sepsis, not uncommon when patients require deep sedation and chemical paralysis to maintain organ function. Even with medication and support, Tinslee has ‘dying events’ 2-3 times per day. When she is in distress, Tinslee crashes and aggressive medical intervention is immediately necessary, which causes even more pain.”
Tinslee Lewis Is Reminiscent of Charlie Gard
Tinslee’s mother spoke with dismay after the ruling, saying she is “heartbroken over today’s decision because the judge basically said Tinslee’s life is NOT worth living. I feel frustrated because anyone in that courtroom would want more time just like I do if Tinslee were their baby. I hope that we can keep fighting through an appeal to protect Tinslee. She deserves the right to live. Please keep praying for Tinslee and thank you for supporting us during this difficult time.”
The case is reminiscent of Charlie Gard’s story. Gard was born in the U.K. with a need for life-extending care. While his parents were hopeful and medical professionals outside the U.K. offered alternative care to that from the National Health Service, Gard’s doctors declined to let his parents take him elsewhere. While this is extreme, it is not too far on the horizon for the U.S. health care system once doctors and judges can determine a patient’s fate rather than the patient or their families.
Tinslee’s doctors argue that she is in pain and this suffering is reason enough to allow her life to end. But determining the value of a life based on the perceived suffering of that person who cannot speak, and whose family wants desperately to keep her alive, is a mistake. While older, terminally ill patients at the end of their lives have more options and have had a lifetime to decide what they would choose when the worst comes to pass, the consideration for the youngest among us must be different. Parents should be the people responsible for making those determinations, and if courts and doctors can take that power away, there are risks for all of us who enter the medical system.
Why Are Doctors Refusing Care?
Not long ago in the United States, hospitals provided no care for premature babies. “The majority of American hospitals had nothing to help them. No technology, no special skills. There was no central heat to keep them warm. Doctors would place heated bricks in cribs and cross their fingers,” said reporter Katie Thornton in an episode of “99% Invisible.”
Treatment for premature babies didn’t begin to change until a doctor in France came up with the idea to house premature babies in something like the incubators used to hatch chickens. The life-saving incubators were not even adopted in hospitals, but first featured as part of a sideshow exhibit at the Omaha World’s Fair and other fairs, hawked on the midway.
Instead of bringing preemies to hospitals, parents would bring them to the fair and hope for the best. These incubators turned out to be the most substantial treatment innovation for premature babies. It was still decades before hospitals adopted the idea and turned it into the concept of the neonatal intensive care unit, or NICU.
Why, now that doctors can do so much, are they turning their backs on the patients that need them most, and saying it’s for their own good? Is it ever compassionate to end a human life if it can be saved or extended, especially in cases where the person is not capable of consent? Tinslee’s mother is hoping for a miracle. In the absence of that, Trinity Lewis would like just a little more time with her daughter. No judge, doctor, or law should stand in the way of that.