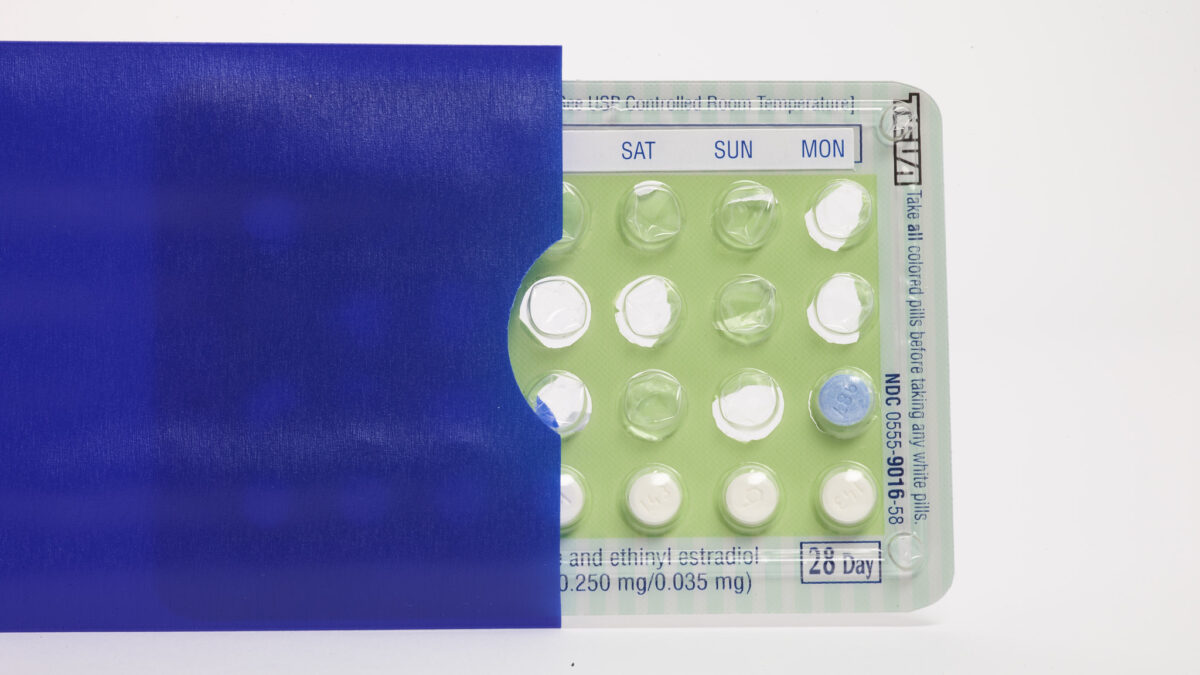
The facade of “safety” around hormonal birth control continues to crumble: Researchers at Oxford Population Health’s Cancer Epidemiology Unit have recently shown that progestin-only hormonal contraceptives, long billed as the “safest” birth control option because of their lack of estrogen, definitively raises one’s risk of breast cancer, similarly to combined hormonal contraceptives (which contain both synthetic estrogen and progestin).
Furthermore, the Oxford researchers found that breast cancer risk, while it declines after discontinuation of hormonal birth control, still remains elevated for ever-users of hormonal birth control (when compared to never-users). Of course, the Food and Drug Administration (FDA) still won’t cop to increased risks for breast cancer for ever-users of birth control — just for current users — and they are also currently evaluating whether to make a progestin-only pill the first-ever over-the-counter birth control pill in the United States.
Unsurprisingly, in another instance of “nothing to see here, folks,” headlines abounded with the results of the Oxford study for a few weeks, carefully emphasizing the “slight” or “small” increase in breast cancer risk. And the experts, of course, were quick to chime in with all the benefits of hormonal contraception, insisting women shouldn’t see this as a reason to go flushing their pills.
ABC’s Chief Medical Correspondent Dr. Jennifer Ashton had this to say, for example:
So listen, I talk to women about this every single day. You have to talk about risk vs benefit. It is clear that hormonal contraception lowers the risk of ovarian and uterine cancer, but it increases the risk of clotting. When you put that head to head, it’s about individualizing that risk-benefit and option-risk for the woman. If you talk to any OB/GYN, they will say, we have a line, ‘pregnancy is much higher risk than any associated risk with birth control pills or hormonal contraception.’ So you have to have that conversation based on you and your health-care provider.
While I agree that health-care decisions should be made between a woman and her doctor, is it really true, with everything we know about the risks and side effects of birth control (and we know an awful lot), that it’s really that much “safer” than a nine-month pregnancy? Women, after all, tend to be on birth control for years — perhaps even decades — at a time. And the oft-touted benefits of hormonal birth control reducing ovarian and uterine cancers? Well, Dr. Ashton might be surprised to learn that pregnancy has those, too.
It’s also worth mentioning that while ovarian and uterine cancers can undoubtedly be devastating diseases, the average woman’s baseline risk for breast cancer is far greater than her risk for ovarian or uterine cancer; in fact, breast cancer is now the world’s most commonly diagnosed cancer. In other words, elevating the average woman’s risk of breast cancer even a little bit should be a serious consideration for doctors and health-care institutions indeed. In fact, one might argue they have a moral imperative to help women lower their risks for breast cancer.
Unfortunately, despite increasing, high-quality evidence of the harms of birth control (of which breast cancer is only one among a lengthy list of risks), health-care organizations such as the FDA are loath to give women true informed consent about these drugs. In 2019, the Contraceptive Study Group (CSG) submitted a Citizen Petition to the FDA requesting they add a black box warning to hormonal contraceptives given the mounting evidence for breast cancer risks for ever-users of these drugs (evidence the Oxford study has yet again corroborated).
Yet in a partial response to the CSG’s petition, published a full three years later in 2022, the FDA refused to supply women with this warning. One wonders what leg they have to stand upon now, and if they’ll continue to ignore these significant risks to women — which can be entirely avoided through the use of highly effective, drug- and side-effect-free measures for family planning known as fertility awareness-based methods.
With the publication of the Oxford study, the FDA has once again proven itself at odds with the best scientific evidence on this matter, which even the National Cancer Institute acknowledges. Again, this is largely because of the “benefit” of preventing pregnancy, which evidently trumps all other considerations — even ones that could take the lives of women.