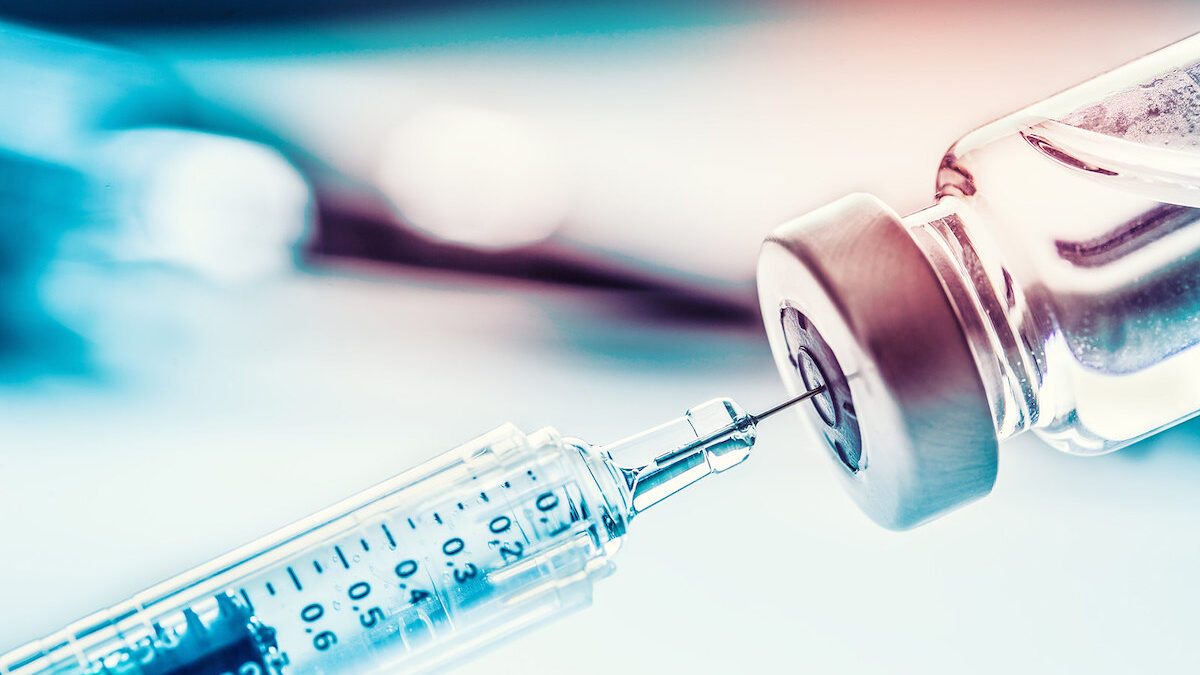
Vaccine-hesitant medical staff across the United States are facing a dilemma: They must choose between what they think is best for their health and their jobs, as already understaffed hospitals begin to mandate the COVID-19 vaccine for all employees.
After a federal judge tossed out a lawsuit from 117 employees at a Texas hospital who wanted to dispute the Houston Methodist Hospital’s COVID-19 vaccine mandate, 153 employees walked out or were fired following a two-week suspension imposed on those who refused to get the shot.
Now, as dozens of hospitals across the country are beginning to require employees to get vaccinated despite pushback from employees and some state governments, those who don’t comply with recently updated Centers for Disease Control recommendations and Federal Equal Employment Opportunity Commission regulations risk losing their jobs, a likelihood U.S. District Judge Lynn Hughes made clear in his ruling.
“Methodist is trying to do their business of saving lives without giving them the COVID-19 virus,” Hughes wrote in his five-page decision dismissing the plaintiffs’ concerns that being fired over the vaccine could be considered “wrongful termination.” “It is a choice made to keep staff, patients, and their families safer.”
This ruling, however, appears to be the beginning of what could be a long fight between healthcare workers, states looking to weigh in on the “vaccine passport” debate, and the hospitals that need them to help keep people alive.
“If mandated in my company, I would be forced to quit at this time,” a female nurse in Florida told The Federalist. “No job is worth my overall health and safety. I worked throughout this pandemic and was not as afraid as I am of this.”
Health-care workers may be hesitant about the vaccine for a wide variety of reasons. Whether it’s the shortened emergency approval period by the Food and Drug Administration, concerns that not enough is known about the experimental vaccines yet, feeling like a “human guinea pig,” as the lead plaintiff in the Texas lawsuit put it, or distrust in the system and people who repeatedly manipulated public panic to push a political agenda, vaccine concerns are alive and well among health workers. Even those who don’t consider themselves “anti-vaxxers” are still struggling to come to terms with how to evaluate the potential risks of the COVID-19 vaccine.
“This I feel is one case where we are the test subjects,” the Florida nurse said. “It is an experimental, emergency authorized vaccine — not something that should be mandated at this time. I have weighed the risk and benefit for my family, and it is just not something I’m comfortable with. Given the limited time and testing, we do not know what effects it will have long term. I’m 50, but my children are 24, 20, and 18. That’s a long life of possible ramifications. To change my mind would require more time, testing, and transparency.”
Others cite the politicization of COVID-19 and the conversation about vaccines as their cause for concern.
“The minute COVID became politicized and doctors began ‘weighing in’ on every news channel like politicians, they could no longer be trusted. Science and politics should not be bedfellows,” a male nurse in Texas told The Federalist. “Even if I was faced with possible demotion or termination, I would still not get the COVID-19 vaccine.”
Nurses’ willingness to speak up about their concerns is repressed by the rising chance of mandates in their industry and peer pressure from colleagues who often make “indirect” and belittling comments about people who are not immediately jumping into COVID vaccination.
“You hear them say, ‘People are so stupid. They don’t understand the science. There is no risk involved at all,’” a female nurse practitioner in Texas told The Federalist.
Not only does demeaning chatter at nurses’ stations make some vaccine-hesitant workers nervous about scrutinizing the COVID shot, but they are also faced with pressure from health-care providers and medical groups such as the American Medical Association and the American Nurses Association to get the shot and even push the vaccine on patients.
“It is the patient’s choice,” the Texas nurse practitioner said. “I can say this is what the CDC recommends … but I definitely don’t push it on people.”
Shortly before the COVID-19 vaccine became available to health workers, polling showed that just above 35 percent of nurses were willing to tell pollsters they would not voluntarily get the shot. While polling six months later shows that more medical staff are getting the vaccine than ever before, the shot mandates do raise questions about whether an exodus of workers who choose to prioritize their health over their jobs will leave hospitals severely depleted of the staffing they need to continue.
After a year of medical chaos, hospitals in California, New York, Florida, and other states are suffering staff shortages that could prove deadly to patients who do not receive good and timely care. If hospitals are unwilling to work with their employees who don’t wish to receive the vaccine, this nationwide understaffing could be exacerbated and cause more lives to be lost as nurses and other medical professionals choose to walk away.
“Do you not work at all? Do you get out of your profession? It’s a hard decision,” the nurse practitioner said.