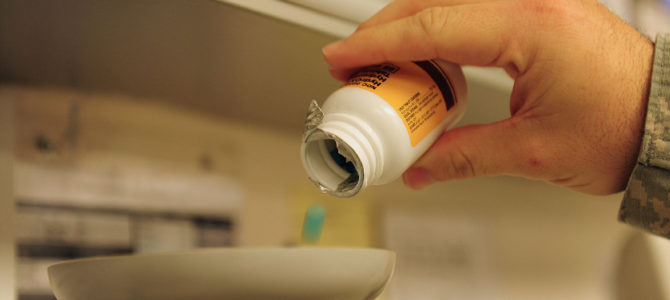
Health professionals and the Trump administration have declared opioid abuse a national epidemic, a crisis of epic proportions that is no respecter of race, class, education, or ethnicity. The National Institute on Drug Abuse reports more than 100 people die from opioid overdoses daily, and it is a “serious national crisis that affects public health as well as social and economic welfare.” The Centers for Disease Control and Prevention estimates the total “economic burden” of prescription opioid abuse is $78.5 billion a year in the United States.
We’ve heard the heartbreaking stories. Recently a young mom who was addicted to opioids overdosed and died, leaving a child behind. The family’s raw obituary, which repeatedly called on the government and “the system” to do more, was touching and difficult to read. President Trump signed a bipartisan piece of legislation Wednesday that, among other things, makes it harder for illicit drugs to be sold.
The question remains: How does an average person get hooked on a drug to the point that he or she overdoses and dies? How can someone trapped in this addiction break free? Can the government really help addicts? I spoke to a former opioid addict to understand his story and find answers to these questions.
The Addiction Begins
Tony Cronen was living in the Twin Cities in 2011, happily married to a beautiful woman named Kim and working as a paint contractor. At 28, Cronen only had one problem. He knew how to solve it. Once he did that, he thought, life would be good. Despite his age, he was significantly and stubbornly overweight. After years of yo-yo dieting and other measures, Cronen decided to take the plunge and have gastric bypass surgery. But the surgery didn’t go well.
Due to severe complications, Cronen nearly died. Following the surgery, doctors had to induce a coma to keep Cronen’s abdomen open to repair leaks and other issues related to the surgery. Cronen had never felt so much intense pain in his life. It was all over his body, but particularly in his limbs.
In striving to keep his vital organs going, Cronen’s body had instinctively ignored his limbs, so he eventually developed neuropathy — a stinging feeling in his hands and feet that is strangely searing and painful. Doctors gave him a narcotic in the hospital, Dilaudid, to help with the pain.
It did help, so he asked for more. Since his body was clearly stressed and his nerves were frayed, physicians gave him more each time he asked. He was in the hospital for eight months.
“I didn’t know it was the beginning of my addiction,” Cronen told me over the phone. But it was. This led to an opioid addiction that lasted several years, nearly destroying his family and his life.
More Pain, Then Rock Bottom
Although it took years for Cronen to realize he was an opioid addict, his failed gastric bypass surgery and the subsequent pain and prescribed narcotics propeled him down this path for several years. That path only led to more pain, more addiction, and finally, rock bottom.
After he was released from the hospital in 2012, Cronen got off the narcotics for three weeks, but had so much pain he went back to the doctor and asked for another prescription.
“I told the doctors, ‘the amount of pain I have is preventing my ability to recover,’” he recalls. So he was prescribed the usual: Oxycodone and then Oxycontin, and finally Hydromorphone, which is the same thing as Dilaudid — all narcotics. “I used it up and asked for more and doctors prescribed it,” Cronen told me. When he eventually ran out, he was told to go to a pain clinic.
It is common for many people hooked on opioids to tell a similar story of pain — from a car accident, surgery, or other chronic issues — that led to narcotic prescriptions, then addiction. The Mayo Clinic details how opioids affect the mind and will convince the body it is in pain to get more of the drug, even when the body is not in pain:
Opioids trigger the release of endorphins, your brain’s feel-good neurotransmitters. Endorphins muffle your perception of pain and boost feelings of pleasure, creating a temporary but powerful sense of well-being. When an opioid dose wears off, you may find yourself wanting those good feelings back, as soon as possible. This is the first milestone on the path toward potential addiction.
Back in 2012, when the nation was just on the precipice of a national crisis of opioid abuse, many pain clinics would prescribe more narcotics, but only until a certain point. Eventually though, Cronen began to game the system. Cronen would take more pills than prescribed, then go to the Emergency Room on the weekends and beg for more.
He usually got them, although he was only supposed to get prescriptions from the pain clinic he was attending and only through one pharmacy at a time. At one point he was taking six 5-mg doses of Oxycodone — nearly quadruple the amount the average person recovering might be prescribed.
“You end up having to take more and more to get the same feeling,” he said. “You use your prescription way faster because two feels better than one and three feels better than two.”
He described the feeling this way:
You feel like you are melting. You don’t care. You don’t care you can’t walk. You don’t care you are in pain. You don’t care you are in the hospital. It is that feeling that gets you hooked. You get so used to not feeling that when you are back in the real world when the drugs are worn off it’s like this onslaught of emotion and you get anxious.
Cronen was kicked out of the first pain clinic — and three subsequent clinics — because he kept abusing the system. Just before he was kicked out of the last one, they gave him a prescription of Hydromorphone that was supposed to last a month. He downed the entire bottle in a week. That’s when he hit his breaking point.
“I had run out of drugs,” he told me. “It was three weeks before my next refill. I had gone a couple nights not sleeping because I was going through withdrawal. I got a bottle of Jim Beam and drank the whole thing. I just wanted to sleep. My wife Kim found me laying in my own vomit. ‘I’m taking William (8 years old) and we are gone,’ she said. ‘I’m leaving you. If you fight me, there’s no chance you’ll get our son. It’s either us or the pills.’”
It had been four years since his surgery, and his wife of nine years was leaving him. He was at rock bottom.
Breaking the Addiction
With his wife’s ultimatum lingering over him, Cronen vowed to break his addiction and heal.
He phoned his younger brother, Aaron, who immediately flew out to be with him. While Cronen quickly dealt with the physical symptoms of withdrawal, which took about three days, the emotional and mental withdrawal from the drugs that had offered so much comfort for so many years was much more difficult to combat. For a year, Cronen staved off anxiety and other effects, but he nearly gave in.
“There were three times I called the pain clinic and made an appointment, and an hour later had to cancel,” he recalled.
However, as the dependency on opioids faded from his mind, he began to realize the negative effects the drugs had on his behavior. This motivated him to stay clean. The drugs had so intensely impaired his own view of himself, he had not realized how awfully he had behaved towards those he loved.
“Once I got off the drugs, I realized what a crappy person I was,” he said. “People don’t realize how drugs change you. People around you know it. But drugs rob you of your personhood. They rob you of your personality.”
One way to explain it Cronen says, is to think of it this way: “When I had legitimate pain, it was excruciating, and I would take these drugs, and they didn’t take the pain away. I could still feel the pain. I just didn’t care. If I didn’t care about that, how could I care about how I was treating my wife or anything? It’s sad to say, but it was the reality.”
Cronen wholeheartedly believes his addiction would have led to his death, had he not stopped sooner.
Labeling the crisis as a national epidemic is an important step, but actually solving it is much more difficult. Cronen isn’t sure what the government could do to really help addicts like him. No amount of programs or self-talk helped heal Cronen. He conquered addiction due to his faith and the presence of people in his life who placed firm but loving boundaries between them and his addiction.
The only thing he thinks could have helped sooner was if physicians and clinics had been aware of the effect of opioids on the brain and never prescribed them in the first place. He isn’t alone in this suggestion.
Still, Cronen has been sober for three years now, and while there have been some effects, he has not looked back to narcotics for comfort. He has no pain from the neuropathy. Slowly, his relationship with his wife began to heal, and he credits the people who love him with helping him finally break his addiction.
“Without my wife and without my faith, I would not have been able to get past it,” he said.