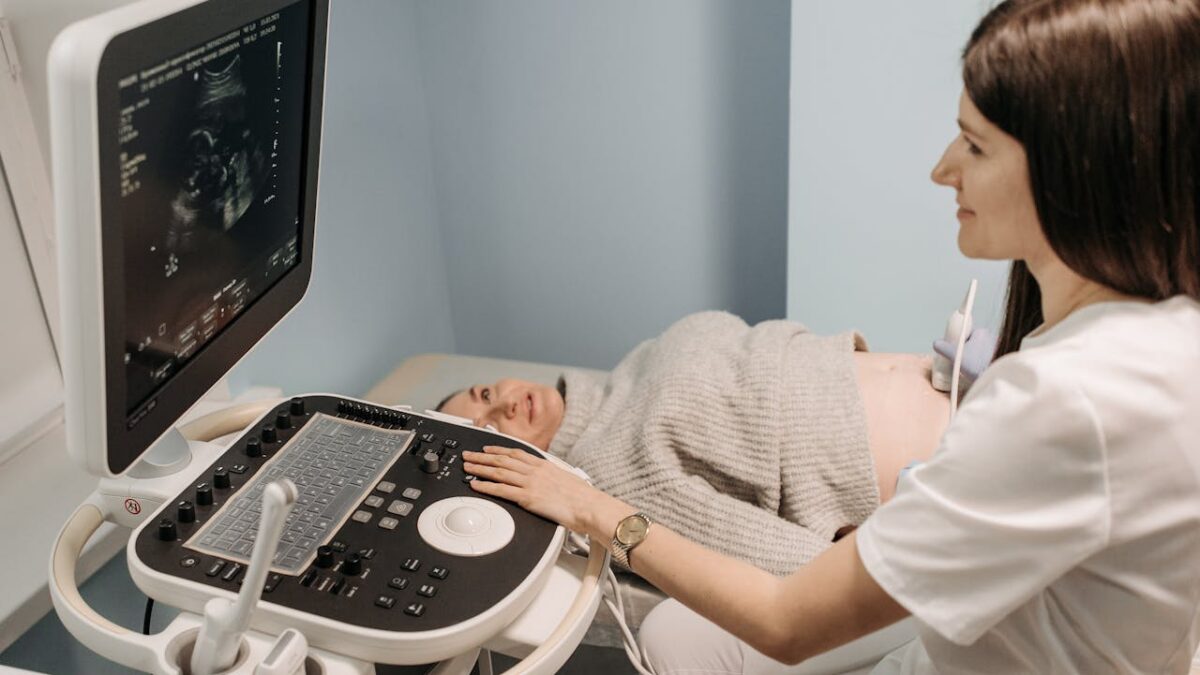
I will never forget it. I answered the phone one June morning in 2009. The voice on the phone said, “If you want to see your mother alive, you will come see her in the next few days.”
A doctor was calling from Washington state and explained that my mother, who was in her 60s, was in the final stages of chronic obstructive pulmonary disease. He gave her literally days to live.
Two days later, I was on a plane from New York to Tacoma. I went to see my mom, who was still in her apartment, since she said she wanted to die at home. She rallied while I was there, and was almost her normal self. A few days later, I went home, but asked her doctor and home health agency to keep in close contact with me.
About a month later, her health took a downward spiral. Her doctor was convinced she was definitely in the process of dying, so we agreed to put her in a hospice facility, since she could not receive hospice care in her own place. Mom was put on painkillers to make her comfortable. I expected that she would be there for a short time, then die peacefully.
That did not happen. Each time her grandchildren came to see her or I called and talked with her, she rallied again. Staff were amazed. Still, after six months, mom’s health did indeed take a turn for the worse and the doctor again said her body had begun the process of dying. My mother decided to go back home to Colorado to die. With agency help, we found her a place and she took the train, which is amazing given how ill she was.
Back in Denver, mom settled in and waited to die. But an odd and wonderful thing happened — she did not die. She eventually found a doctor who adjusted her medications and oxygen and took her off of all of the heavy pain meds. She got a new wheelchair and began to venture out into the community. Before long, she was back doing what she loved—volunteering to advocate for people with disabilities. Weeks after her return home, she traveled to Washington DC to help fight for disability rights.
Terminal Illness Diagnoses Are Sometimes a Mistake
My mother’s story illustrates how doctors can and do make mistakes when they determine that someone is terminally ill. More than seven years have passed since that morning in June when I was first told my mom was dying. Happily, she is still alive. Her health isn’t the best, but she is still in her own place and still reasonably active in the community.
What happened to my mom happens far more often then we realize. It’s one reason assisted-suicide laws are so dangerous. Eligibility for assisted suicide typically depends on a doctor’s prediction of death within six months. Distress over receiving that kind of bad news could lead someone to make a hasty exit and, potentially, miss good years of life.
Fortunately, my mother, who often jokes that she’s too ornery to die, wasn’t the kind to contemplate checking out early. But when she lived in Washington state, all she would have had to do was ask and sign a form and she would have been given lethal drugs.
Some people say that’s her choice. If they were talking about suicide, that’s true. But they’re talking about doctor-assisted suicide, and that’s the doctor’s choice, along with any others who may be involved, whatever their reasons may be. That’s where there’s plenty of room for concern.
These Laws Particularly Prey on the Vulnerable
Most people of color are against doctor-assisted suicide. Studies show that blacks are treated differently than white patients and receive inferior care, particularly in cardiac care, diabetes, and pain management. Blacks are more likely to die because doctors have overlooked something critical or will not listen to or believe what we have to say about our health and pain. Also, because we’re more likely to be poor, we are at greater risk of being persuaded or coerced by doctors into assisted suicide, citing the financial burden we’d be to our family.
Data from Oregon and Washington shows that people request assisted suicide mainly for psychological and social reasons. Healthy, nondisabled people get support to live when they express suicidal feelings, while people who are sick and disabled, particularly those deemed terminally ill, get suicide medication. Why not suicide prevention, pain relief, and home care? Would that be so difficult?
Or is the difficulty and cost of quality care the real issue? A particularly frightening reality is that some insurance companies in Oregon and California, where doctor-assisted suicide is legal, have begun denying cancer treatment to patients, opting instead to pay for lethal drugs. This is not the way society should respond to human beings’ needs for health care.
Assisted suicide laws are a bad prescription. We shouldn’t take it.