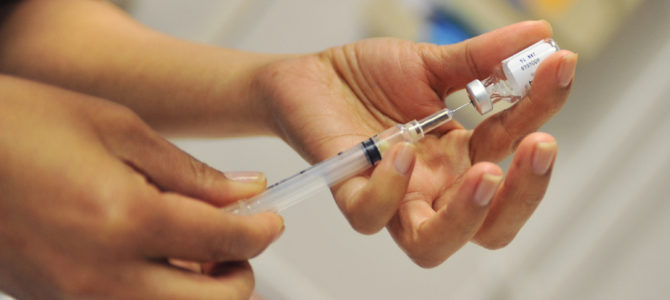
It is widely agreed upon in health care that immunizations are the second greatest advancement in public health—only behind clean drinking water. However, despite the known success of vaccines in reducing morbidity and mortality, immunization rates remain relatively low across the United States, especially in the 19- to 35-month age range.
But Americans who blame anti-vaccination parents and propaganda have it wrong. Yes, those who do not vaccinate their children play a role in our failing rates, and lies about vaccinations causing autism have made matters worse, but there are less known, more significant causes to poor completion rates in children. Those are primarily time and money. Low immunization rates are the result of a misaligned financial incentive structure for vaccination providers transferred to parents.
19 Shots Is a Lot to Pay For
Parents have a lot of choices to make. There are cost-benefit analyses to be done that include weighing vaccination risks such as allergies, as well as an intensifying mistrust of the traditional institutions in the United States. But there is also a growing need to recognize that as the world globalizes, travel increases, and bacteria evolve, herd immunity is vital for children’s safety.
Sadly, this has become more difficult as the number of recommended vaccines has increased from 10 doses in 1983 to almost 30 doses in 2015—each with an individual monetary and time cost for parents. For example, the conventional model for dispensing vaccines includes: four DTap, three polio, one MMR, three Hib, three Hep B, one varicella, and four PCV (4:3:1:3:3:1:4), for a total of 19 antigens being administered. Using traditional, monovalent vaccines, these 19 antigens are administered via 19 separate shots, and thus 19 separate fees.

Unfortunately, as the number of recommended childhood vaccines has nearly tripled, the likelihood of on-time and successful completion of vaccination series is reduced. Further, families living below the poverty line are less likely to complete their vaccination series due to the added financial and time constraints.
So, Combine the Vaccines
This begs the question, why don’t doctors use combination vaccines? Combination vaccines take two or more vaccines that could be given individually and merge them into one shot. The sad answer is that doctors are not financially incentivized to. Vaccinations make doctors almost no money, and therefore the more shots they give, the more money they make. This is the exact problem health care faces in so many areas that reimburse using a fee-for-service model. It is also a barrier to achieving higher vaccination rates.
Although the Affordable Care Act attempted to address the issue of misaligned payments by increasing primary care Medicaid vaccine reimbursements, both Medicaid and private insurance still make earnings for doctors who administer vaccinations almost impossible. For example, reimbursement for Medicaid vaccine administration varies by state, but it’s as low as $2 in some states, often leaving providers with a net loss for administering a shot. Further, study findings note that 10 percent of family physicians already do not give vaccines to children, and another 10 percent are seriously considering discontinuing childhood vaccination because of costs.
At present, using combination vaccines, the recommended antigens for children could be administered in as few as 13 shots, saving parents lots of time and money. However, because doctors would lose even more money administering fewer vaccinations, there is no reason to make parent’s lives easier.
The saddest part of the misalignment of incentives is that children are the ones who suffer. Low reimbursements mean doctors’ lives have more difficulty making ends meet while doing their jobs, and parents’ lives are made harder by trying to stick to the government-proposed (and sometimes mandated) schedule at higher costs.
Using combination vaccines has been endorsed by the Advisory Committee on Immunization Practices (ACIP) and Centers for Disease Control (CDC) as a safe and efficacious way to decrease the number of injections needed to complete the childhood immunization schedule. Additionally, combination vaccines have been shown to enhance immunization rates and timeliness of vaccine delivery.
As such, the CDC, the American Academy of Family Physicians, and the American Academy of Pediatrics strongly recommend children receive combination vaccines whenever possible to improve completed vaccination series rates for children. It’s time to recognize the significant and detrimental role monovalent shots are having on America’s youth, and properly incentivize doctors—and parents—to vaccinate children to the best of their ability.









