Social media overflowed this past week with heart-wrenching testimonies of “justified” later-term abortions, following Hillary Clinton and Donald Trump’s comments on the topic during their third presidential debate. One woman wrote for the New York Times that “Late-Term Abortion Was the Right Choice for Me.”
But these opinions are not new: as a mother raising a child diagnosed in-utero with a critical Congenital Heart Defect (cCHD), this is a narrative I have looked square in the eye—and rejected—time and time again.
They are the same stories and opinions I encountered from the first days after receiving my son Walter’s diagnosis: from my maternal fetal specialist, from chat rooms, and from any quick google search of Tetralogy of Fallot with Pulmonary Atresia (ToF with PA). Though the above New York Times article refers to a baby likely diagnosed with Hypoplastic Left Heart Syndrome (HLHS), mothers receiving these diagnoses face a similar tragic reality: in a medical community saturated with abortive answers to imperfect realities, somewhere north of 75 percent of babies with critical CHD will be “terminated for medical reasons” prior to birth.
How We Learned Our Son Had a Congenital Heart Defect
These various abortion stories are often powerful because they reject the pro-life narrative that aborted babies are unwanted from the beginning. Though a human heart is formed between weeks five and six of pregnancy, defects are often not noticeable or not examined until the standard week 20 anatomy scan. This means a mother is often visibly pregnant. She has felt her child move, may already have had a baby shower, or decorated the nursery. In many cases, these families name their baby, have postmortem photos taken together, and hold a memorial service.
I pray for these women, because they acted out of what they thought was mercy for their child. They trusted medical providers who made them feel that life with an imperfect heart (needing painful open heart surgeries and the uncertainty of transplants) is not a life worth living. Because our society and culture has told them that an imperfect life is a valueless one. Because women (as well as their unborn children) have been let down by a country that will fight to not simply permit abortion, but celebrate it.
My position is not a popular one among many of my friends and some extended family. But legality and right aside, let us at least discuss this “choice” given to women in the wake of these diagnoses. Quite possibly, we may have something to agree on.
First, I’d like you to step into my shoes for a moment: 22 years old, newly married, and pregnant with my first child. I had just moved to a new state, far away from family, to support my husband in his career as a Marine—a duty that keeps him away from home 50 to 75 percent of the time. I had just started a new job with great pay and good benefits, and was part of a fast-track program to high-level management positions within a Fortune 500 company. It was also a job wherein I would soon use all my sick time and vacation going to doctor’s appointments, begin my FMLA early, and later resign, unable to keep up with the demands of work and the extensive prenatal care we needed for our son.
My situation was never desperate. It was happy, beautiful, and full of life’s challenges, but given the news we would soon be given about Walter’s heart, many would not fault me for taking “mercy” on my child and ending his life prior to his birth.
We Were Pressured to Abort Our Baby
The narrative I have shared with family and friends regarding my son’s diagnosis has always been a hopeful one: one in which my husband and I had everything together and expert doctors were planning to save Walter’s life. But there has also always been so much more to that story.
We glossed over the part where our maternal fetal specialist handed me a box of tissues and said things didn’t look good—that our son may not survive birth—and if he did, he would have a tragic life. The part where “termination” was brought up multiple times, but no mentions of adoption ever discussed. The part where open heart surgeries were broken down into terms like “bypass time,” “heart stopped,” “your child’s body on ice,” “intubation,” “unable to breath,” and “mortality rates.” Hope of success and promise for our son was reserved until long after his diagnosis—after we had already decided to fight for him. Our already-named son was referred to as only “the fetus.”
There was the time I slept on the floor of Walter’s painted and decorated nursery for a week, believing in my heart that he would never come home to enjoy it. The time my strong, steady husband’s eyes welled up and his voice shook when he said “brain and heart anomalies.” The time he was quietly asked to leave the room, so that I could sign consents acknowledging that I had been advised of (and declined) my abortive rights in the state of Virginia.
I am grateful I have a husband (and family, and faith) that values the life of the unborn, prior to ever learning about Walter. I am grateful that my husband Dan and I discussed before getting married (let alone pregnant) that regardless of what any prenatal testing might show in any child we had, we would do everything in our power to help that child live—and at the very least, be born. The cruel reality is that Walter’s heart was made to fail, and it is only through the miracle of modern medicine that he had a chance to live beyond a few months old.
Many Mothers Aren’t Told That Life Is Truly An Option
But I also know that many women do not have this support system. They don’t receive information or resources. In one of their most desperate and vulnerable moments, they turn to their doctors—who greatly favor termination over palliative care (as there is, of course, no cure for CHD). They turn to doctors who give no information about adopting out a child with complex medical needs to a family prepared to handle them. They turn to doctors who refer them to cardiac specialists only after rejecting termination as an option.
When I was handed information on ToF w/ PA, there was a simple medical description of the diagnosis describing the four-part defect (five including the Pulmonary Atresia), and a notice of my abortive rights in the state of Virginia. No adoption pamphlets, no CHD support group information, no contacts of local parents raising a child with CHD who may be able to provide some answers. No hope.
We were given some resources similar to these through the Children’s Hospital in Washington, D.C. only after deciding not to terminate Walter’s life. Even then, I was not introduced to our “LA Heart Moms Group” until Walter was already in the middle of his first open heart surgery, by another “Heart Mom” who approached me in the waiting room. It was through my own research (hours upon hours of it) that I found personal stories, alternative treatments, research studies, medical journals, and so on. These were not handed to me with the same gravity and authority as the termination notice from my doctor.
Later, after Walter’s birth, we learned of a local family who chose to terminate their child with ToF, and our hearts broke. I contacted our Navy OBGYN clinic to see if perhaps, I could provide them with contact information for our LA Heart Mom Group, so that women given a CHD diagnosis in the future could speak with women who had been in a similar situation. I also asked if the clinic worked with any adoption agencies to offer their services to women considering termination.
I was given a firm “no” and “no.” This reality is true across the medical field: they are bound by strict laws and regulations that prohibit “advocating” this kind of information to their patients.
What Kind of Choice Is This?
After having difficulty conceiving our second child, I quickly began looking into adoption, finding that no networks existed with the purpose of putting women carrying babies with various defects (like CHD) in contact with families specifically looking to adopt children with a certain disability.
Yes, adoption agencies and the foster system exist—but there is nothing as specific or as helpful as what I was looking for. And medical professionals are not allowed to present any of them to the women given these diagnoses. (Of course, a discussion of adoption—its hurdles and expenses—is an entirely separate and tragic discussion on its own.)
What this all leads me to ask is, “What kind of ‘choice’ is this?” What options and support are we truly providing mothers, in a system where terminating a child with birth defects is the primary objective of the medical community? I can only imagine the uproar were the situation reversed. In our society’s attempt to make sure a woman’s right to abortion is protected, we have dismissed her right to fight for her child.
If the Left is earnest about their respect for a mother’s choice—if they look at a room of toddlers and see Walter’s life just as equal and valuable as all the others, despite his critical life-threatening heart defect—then we can agree that medical practitioners should be legally required to provide alternative options to abortion as equal and valuable as termination.
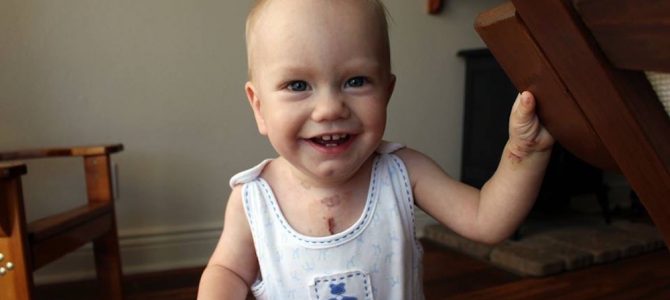
As it stands, when I look at my energetic, curious, and thriving son, I know about half the people he meets would find the prospect of his pre-birth execution not horrific, but understandable. At the very least, I would like mothers confronting the same choice to get more opportunities to see and meet children like our Walter. Just maybe, more children would get to thrive, laugh, and love as a result.