New research indicates hormonal birth control is correlated with depression, and women across the world went, “Tell us something we didn’t know.”
This study from the University of Copenhagen concludes hormonal contraceptive use was associated with higher subsequent use of antidepressants and a diagnosis of depression, especially for teenagers. Compared to women who weren’t on birth control, nearly women using birth control pills were nearly one-quarter more likely to have been prescribed an antidepressant. Teen girls on birth control pills were 80 percent more likely to be prescribed an antidepressant, and teens using non-oral hormonal products saw tripled risk.
The study also notes that doctors, aware hormonal contraception can cause mood changes, are less likely to prescribe birth control to women already suffering from clinical depression. It also finds women are likely to cease using hormonal birth control when experiencing mood disorders without necessarily seeing a doctor or psychiatrist. Therefore, the effect of hormonal pills on depression may be underreported.
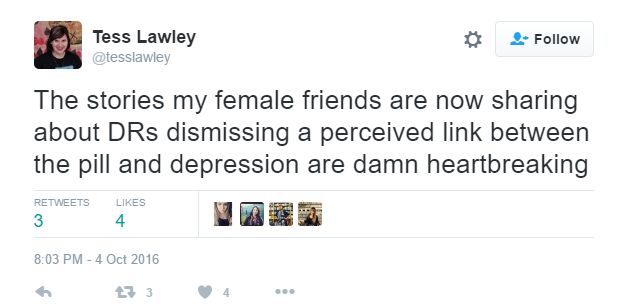
In The Guardian’s report on the study, author Holly Grigg-Spall said, “The largest of its kind, with one million Danish women between the ages of 15 and 34 tracked for a total of 13 years, it’s the kind of study that women such as me, who have experienced the side-effects of birth control-induced depression first hand, have been waiting for.” It appears to have hit a nerve. Women took to Twitter to express frustration and vindication:
Whether Men or Women Deny These Findings, They Matter
Grigg-Spall is a long-time critic of hormonal birth control and author of the book “Sweetening the Pill,” which is now being turned into a documentary (co-produced by none other than Ricki Lake). She went on to rage against “pillsplaining” from medical professionals who continued to deny the importance of this study.
She, of course, did not name the researchers and doctors who implied that the study can be explained mostly by “teen heartbreak.” She blamed an industry led by people who do not care about women’s health or experiences, and paternalistic gaslighting from men who have never had to take the pill. This is an unfortunate obfuscation, because two of the most rage-inducing reactions to this study come from women:
“With having a million women, there are 101 things that are variable here…There’s other things going on in their life like relationships, relationships breaking down and especially with adolescents — just being in a sexual relationship,” said Diana Mansour, vice president for clinical quality at the Faculty for Sexual and Reproductive Healthcare in London.
“The possibility that this link between love, sex (contraception), and feeling depressed is strengthened by the fact that the contraception-depression link was strongest in adolescents, those who are at the developmental stage where trying to find a romantic partner is paramount,” said Catherine Monk, an associate professor in psychiatry, obstetrics, and gynecology at Columbia University Medical Center.
Can we stop blaming everything on male attitudes? If it’s indeed misogyny, it appears to be a trait women share. I could posit my own conspiracy theories about how making hormonal birth control seem dangerous to the general public may send women’s liberation back a few decades, which indeed feels threatening to the women who fight for sexual freedom.
Please Don’t Dismiss Depression; It’s Really Serious
Personally speaking, the study seems rather legitimate. The researchers even considered “teen heartbreak,” so to speak, as a confounding factor, and therefore restricted their analysis to women who mostly had already had their first sexual intercourse.
Certainly that does not completely eliminate the heartbreak factor and the generally turbulent nature of adolescent relationships, but it does help in gathering women who are slightly more experienced in romantic entanglements. The MGH Women’s Center for Mental Health likewise posited this sample of older women was naturally restricted, as it may have been harder to find women of that age who had not already had a depressive episode and were still affected for the first time by the pill. That center acknowledged the study shows a small but statistically significant correlation between hormonal birth control and the risk for depression.
It’s already well-acknowledged that depression can be affected or even caused by estrogen and progesterone imbalances. My personal experience fits that narrative. Ironically, it was the pill (Yaz, to be exact) that first helped balance my mood, as it was prescribed to combat Premenstrual Dysphoric Disorder (PMDD, the more severe form of PMS).
Later experiences, including two very healthy, happy, and glowing pregnancies followed by two disastrous postpartum experiences, cemented for my doctors and me that I am extremely susceptible to reproductive hormones. I have often joked that my body was designed for pregnancy: my mood changes based on my reproductive cycle, and I have been happy and medication-free during all three of my pregnancies, including this current cycle of being pregnant. The irony, of course, is that the newborn period destroys me, and breastfeeding appears to exacerbate my depression.
Of Course Hormones Affect Women
Irony aside, truly understanding that women can be so severely affected by hormones, whether natural or artificially generated, is freeing. It should be an obvious observation. However, I share many women’s frustrations about not being taken seriously when trying to understand the link.
My second attempts at birth control, after I had experienced postpartum depression, plunged me deeper into the hole. Therefore, I now know to explore non-hormonal options, such as natural procreative technology, copper IUDs, or barrier methods. My joke that I love being pregnant has led me, similarly, to explore bioidentical hormonal replacement therapy (often used for menopausal women) to combat depression in order to stave off using my non-breastfeeding-friendly anti-depressant.
Look. Pills aren’t bad, including hormone-based ones. I hope to use those same hormones—a progesterone shot right after birth—to avoid the need for my literally life-saving depression medication. My first experience with hormonal birth control, similarly, increased my quality of life. Artificially-provided hormones can help, hurt, or have no effect on any given woman.
However, the reason this study is resonating with so many women is that despite the oft-repeated stereotypes of women being “hormonal,” practitioners don’t appear to take women seriously when they look for advice on the effects of those hormones, and often dismiss those who truly appear to have issues with the hormones being pumped artificially into their bodies.