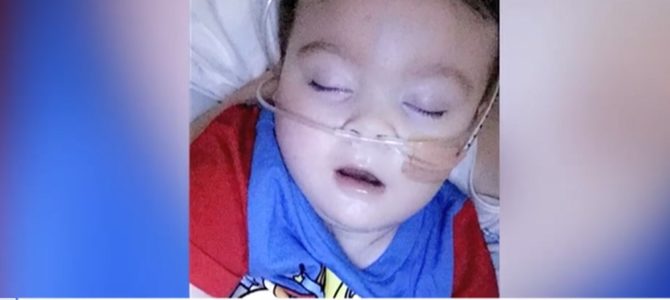
Once again, a single-payer health-care system has attracted international attention for its moral depravity. The case concerns Alfie Evans, a British toddler who, by virtue of his slim chance at survival, is barred from seeking treatment elsewhere that might well save his life.
Appropriately, opponents of single-payer health-care have seized on Alfie’s case as an example of taxpayer-funded medicine’s evil nature. In response, single-payer advocates have asked what the difference is between Alfie and an American who dies because he is too poor to afford the health care he needs.
It’s not an unfair question, and it deserves an answer. To do that, however, it’s important to revisit how a situation like Alfie’s came to be.
Single-Payer Is Limited by Tax Revenue
When a nation enacts universal, taxpayer-funded health care, it effectively builds a wall around its health-care system. Within this wall, resources are finite, which effectively creates a zero-sum game where one person’s gain is necessarily another person’s loss (only so much medication may be dispensed; only for so many hours of the day can a doctor spend seeing patients; only so many hospital beds can be vacant).
Where in a free market health system a patient has the entire global health industry at his or her disposal and is limited only by individual wealth, in a public system, a patient has access only to resources the government has acquisitioned and made available for use.
The extent of these initial constraints varies on the type of the system (a single-payer system, for example, will have tighter controls than a government health insurance option), but the underlying forces at work remain the same—namely that people prefer quality in health care for themselves over quantity in health care for the masses.
But preferring oneself in a collectivist health care system is problematic. For example, in a public health insurance model, in which the federal government offers an insurance plan that competes with private plans, doctors will generally prefer the payout of private insurance over that of public insurance. This is hardly theory. According to a 2017 study, in the United States, the average Medicaid acceptance rate among physicians in major metro markets is only 53 percent.
To solve this problem, the government will force doctors to accept a certain quota of publicly funded insurance-holders or restrict access to private insurance altogether. Both options create a de facto single-payer system. The former destroys the incentive to pay extra for private health insurance (chiefly, faster and better care) while the latter simply destroys private health insurance itself.
Offering Unlimited Care Causes People to Use Much More
Regardless of execution, once a government has secured total control over a nation’s health system, it will immediately run into a cost problem. Realizing the enormous fiscal burden that accompanies shouldering an entire nation’s health needs (a nation, mind you, in which individual consumers have no motivation to limit their costs), governments will turn to a mixture of three solutions to reduce spending or increase revenues.
The most obvious of these is to increase taxes. But this alleviates the government’s financial shortcomings only temporarily. A tax plan is only as good as the economy that supports it, and a tax-and-spend plan that excessively saddles a country’s economic engine will ultimately fail. Nowhere is this clearer than in Greece, where public health-care providers have turned to soliciting donations to meet their needs. Even taxing the contemptible “millionaires and billionaires” will provide only short-term relief, if any. There’s simply not enough money there for everyone.
When tax increases inevitably fail to cover costs, the government will adopt a more draconian approach to control spending. Laws will be introduced—like those in Britain—that force doctors to work in the public sector for lower wages. Doctors may be forced to work for free, and despite having obtained years of advanced and highly technical education, will find themselves in wage wars similar to those involving public school teachers.
Understandably, this decline in wages will force some doctors to cease practicing medicine, at least in their home country (see Greece’s “exodus of doctors and nurses”). To be sure, not all doctors will close their doors, but many will—likely enough to exacerbate the already-short supply of doctors, leading to the infamously long wait lines common to all taxpayer-funded systems. A tighter supply of doctors will, by default, increase their demand. Unable to pay doctors their true worth, the government will make a ham-fisted attempt to “reduce” demand—by rationing health care.
Enter Alfie Evans: a toddler destined to die so the government can pay the entire nation’s health bills. It doesn’t matter that Alfie can get treatment elsewhere. It doesn’t matter that Alfie’s parents object. It doesn’t matter that all human decency in the world is screaming in outrage at the barbaric injustice perpetrated by Britain’s single-payer death squads. The sacrificial lamb must be slaughtered in the name of progress.
What, then, is the difference between little Alfie’s case and the case of the poor American who cannot afford the health care he needs? Simple: The American’s life was lost. Alfie’s life was stolen.